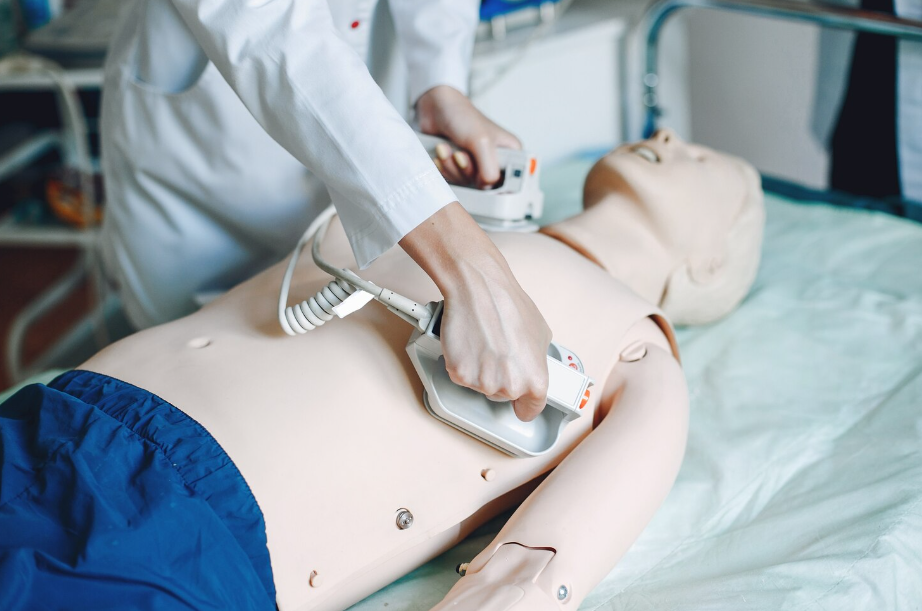
What Is a Defibrillator and How Does It Work
A defibrillator is one of those devices you hope you never have to see in action, but when you do, it can literally save a life. Basically, it sends a controlled shock to the heart if the rhythm goes haywire, things like ventricular fibrillation, where the heart is just not cooperating. Doctors and trained responders use them all the time in emergencies, and every minute really does matter. Survival drops fast if nothing happens right away.
The way it works is simple when you think about it. Pads go on the chest, electricity goes through, and the heart gets this jolt that lets it “reset” itself. It doesn’t magically fix everything, but it gives the heart a chance to beat normally again. When the rhythm is all over the place, blood just isn’t moving right, so this little jolt can make a huge difference.
Of course, a defibrillator isn’t the whole solution. CPR or other treatments usually happen at the same time. And honestly, if someone in your family needs one, it’s really worth talking to a leading electrophysiologist in Los Angeles. They can explain which device makes sense, how it works for that person, and how to keep an eye on it so it actually helps when it’s needed.
Why Defibrillators Save Lives
Time becomes the biggest enemy during cardiac emergencies. When someone collapses from sudden cardiac arrest, their brain starts suffering damage within 4-6 minutes without oxygenated blood flow. Defibrillators bridge this critical gap by restoring circulation before permanent damage occurs.
You’ll find these devices in hospitals, ambulances, schools, airports, and many public buildings. The reasoning is simple: cardiac arrest can strike anyone, anywhere, without warning. Having immediate access to defibrillation dramatically improves survival odds compared to waiting for emergency services to arrive.
Modern defibrillators include voice prompts and visual guides that walk users through each step. This design makes early intervention possible even when trained medical staff isn’t immediately available. Studies consistently show that bystander defibrillation, combined with CPR, can double or triple survival rates.
How Defibrillator Pads Function
The electrode pads serve as the connection point between the device and the patient’s heart. These adhesive patches contain conductive gel that ensures proper electrical contact with the skin. Placement matters tremendously here. One pad typically goes on the upper right chest below the collarbone, while the other goes on the lower left side below the heart.
Good adhesion prevents the pads from shifting during shock delivery, which could reduce effectiveness or cause burns. The pads also feed heart rhythm information back to the defibrillator’s computer, allowing it to analyze whether a shock is appropriate. Different defibrillator models use specific pad types, so compatibility becomes important for healthcare facilities managing multiple devices.
Some advanced pads include built-in sensors that monitor chest compressions during CPR, providing real-time feedback on compression depth and rate. This integration helps responders maintain high-quality resuscitation efforts between defibrillation attempts.
The Defibrillation Process Step by Step
When you encounter someone in cardiac arrest, the defibrillation process follows a clear sequence. After confirming the person is unresponsive and not breathing normally, you’d power on the defibrillator and expose the chest area. Remove any clothing, jewelry, or medical patches from the chest to ensure clean pad contact.
Place the pads according to the diagrams on the device or pad packaging. The defibrillator then analyzes the heart rhythm through these pads. During this analysis phase, nobody should touch the patient since movement can interfere with accurate rhythm detection.
If the device determines a shock is needed, it will charge automatically and prompt you to deliver the shock. Before pressing the shock button, you must ensure everyone is clear of the patient. The electrical discharge lasts just milliseconds but temporarily stops all heart activity. After the shock, the device typically guides you through CPR cycles while continuing to monitor the heart rhythm.
Different Types of Defibrillators
Automated External Defibrillators (AEDs) are the ones you’ll encounter in public spaces. These portable units make decisions about when to shock based on their rhythm analysis. They’re designed for use by people with minimal training, featuring simple instructions and automatic charging systems.
Manual defibrillators give healthcare providers more control over energy levels and timing. Emergency room doctors and paramedics can adjust shock strength based on the patient’s size and condition. These devices also offer additional monitoring capabilities like blood oxygen levels and blood pressure.
Implantable Cardioverter Defibrillators (ICDs) live inside patients who have a high risk for sudden cardiac death. These small devices continuously monitor heart rhythms and deliver automatic shocks when dangerous rhythms are detected. ICDs can also pace the heart when it beats too slowly.
Wearable defibrillators offer temporary protection for patients waiting for ICD implantation or those whose condition might improve with medical treatment. These vest-like devices provide the same monitoring and shock capabilities as ICDs but from outside the body.
Operating a Defibrillator
Turn the device on first, which activates voice prompts that guide you through each step. Most units start talking immediately, telling you to place the pads on bare skin. Follow the placement diagrams carefully since incorrect positioning reduces effectiveness.
Once pads are attached, the defibrillator automatically begins analyzing the heart rhythm. This process takes about 10-15 seconds, during which you should avoid touching the patient. The device will announce whether a shock is recommended based on what it detects.
If a shock is advised, make sure everyone steps back from the patient before pressing the flashing shock button. The device will deliver the programmed energy level, usually starting around 150-200 joules for adults. After each shock, you’ll typically be prompted to begin or continue chest compressions for two minutes before the next rhythm analysis.
Keeping Defibrillators Ready
Regular equipment checks ensure defibrillators function when needed. Most units perform daily self-tests automatically, checking battery levels, charging circuits, and other internal components. Look for status indicators that show green for “ready” or red for “service needed”.
Electrode pads have expiration dates since the conductive gel dries out over time. Replace pads when they expire or if the packaging gets damaged. Keep spare pads stored in a cool, dry place away from direct sunlight.
Battery replacement schedules vary by model, but most need new batteries every 3-5 years. Some units use replaceable lithium batteries, while others have built-in power sources that require professional service. Training records should be updated regularly for anyone expected to use the device during emergencies.
Temperature extremes can damage defibrillators, so storage areas should stay within the manufacturer’s specifications. Regular cleaning with appropriate disinfectants keeps the device sanitary without damaging sensitive components.
Contact Us
At CEPI, we’re always here to assist you. Whether you have questions about our services, need to schedule an appointment, or would like to learn more about cardiac electrophysiology, our team is here to help.
Office Location: 8631 West 3rd Street #710E, Los Angeles, CA 90048
Phone: (310) 746-5335
Office Hours:
- Monday to Friday: 8:00 AM – 5:00 PM
Get in touch today! Prefer to reach out online? Fill out our contact form, and a member of our team will get back to you promptly.
Related Topics: